Chapter 3
The impact of the bills
3.1
This chapter
summarises the evidence the committee has received on the likely impact of the
legislation. It is divided into four sections:
-
the impact of
the lower private health insurance (PHI) rebate and the higher Medicare Levy
Surcharge (MLS) on the financial options for different income groups;
-
the impact on
private health fund membership including Treasury's modelling, objections to
this analysis, and behavioural and historical observations on the factors that motivate
the buying and retaining of private health insurance;
-
the impact on
public hospitals; and
-
the process of
implementing the means tested rebate.
The bills' impact on different income groups
3.2
Treasury
estimates that means testing the PHI rebate will impact 'on around the top 23
per cent' of those with private health insurance.[1]
Within this group, nine per cent (870 000 people) are in Tier 1
($75 000–$90 000), seven per cent (720 000 people) are in Tier 2
($90 001–$120 000) and a further seven per cent (690 000 people)
are in Tier 3 ($120 000+).[2]
3.3
In terms of
the impact of the higher MLS, Treasury estimates that there are currently
310 000 taxpayers who are liable for the surcharge (earning over
$70 000 and without PHI). Of these, 180 000 MLS payers are in Tier 1
and will not be affected by the MLS changes. The higher surcharge will be borne
by the remaining 130 000 MLS payers in Tiers 2 and 3 (those without PHI
earning more than $90 000).
3.4
The committee received some analysis of the likely impact of the
bills' measures on the financial position of those with PHI in Tiers 1, 2 and
3. This indicated that the increase in premiums as a direct consequence of a
reduced PHI rebate will be minimal. Further, the countervailing increase in the
MLS for higher income groups would encourage the uptake of cheap PHI policies.
3.5
In his written and verbal evidence to the committee, Dr John Deeble
downplayed the effect of the bills' measures on PHI premiums. He noted that the
average PHI premium for a family hospital cover policy in 2007–08 was $1905. Based
on past trends, premiums for hospital cover will increase by five per cent over
the three years to 2010–2011, which gives a projected family policy premium for
2010–2011 of $2000. If current arrangements continue, therefore, all those
privately insured with an average family policy would receive a $600 rebate
(30 per cent of $2000) leaving them a $1400 premium.[3]
3.6
Dr Deeble noted that under the bills' measures, those families
earning the midpoint in Tier 1 ($165 000 per annum) will receive a $400
PHI rebate (20 per cent) on a $2000 policy. This equates to an average increase
of $200 a year or only $4 a week. Families earning the midpoint in Tier 2 ($210 000)
will receive a $200 rebate (10 per cent) on the same policy, which equates to a
$400 a year increase in premiums or $8 a week. Dr Deeble concludes:
...for a family earning $165,000 a year, private hospital
insurance would rise by only $4 per week – about the price of one cup of
coffee. For a family with a $300,000 income, it would still amount to only three
cups. It is impossible to believe that such minor changes could ever lead to
the kind of consequences for membership and premiums that the private health
insurers have claimed.[4]
3.7
Mr Ian McAuley, a Fellow at the Centre for Policy Development, extended
this analysis by taking into account both the rebate reductions and the higher
MLS (see Appendix 3). He argued that if people act rationally and are
calculating in response to the bills' measures, two trends would be evident.
The first is an uptake in PHI among taxpayers currently paying the MLS.[5]
The second is a preference for cheaper PHI policies with incentives for all
income groups to drop their ancillary cover.[6]
3.8
Mr McAuley's submission noted that for singles with a relatively cheap
policy ($1000 a year), the current and proposed arrangements offer an incentive
for almost every taxpayer with an income over $75 000 to remain privately
covered. For example, under current arrangements, a single person earning $100 000
a year with a $1000 policy receives a net benefit of $300 from having PHI; the
full extent of the 30 per cent rebate. Under the proposed arrangements,
this person faces a 1.25 per cent MLS ($1250) and a reduced rebate of $100
(leaving $900). The net benefit from having a $1000 policy, therefore, is $350.
Mr McAuley wrote in his submission:
...in effect, both the "old" and "new"
incentives provide free PHI for people with high incomes, with change left
over, and the higher one’s income the greater is the overcompensation.[7]
3.9
Mr McAuley also noted that for singles with incomes between $75 000
and $115 000 per annum (double for couples), there is less incentive under
the proposed arrangements to hold high price policies. Under current arrangements,
a single person earning $100 000 a year holding a $2000 policy faces a net
payment of $400 from having PHI ($1400 after the $600 rebate compared with a
$1000 MLS). Under the proposed arrangements, this person faces a 1.25 per cent
MLS ($1250) and a reduced rebate of $100 (leaving $1800). There is a net
payment from having a $2000 policy of $550.
3.10
Mr McAuley acknowledged that the incentive to hold a $2000 a year policy
increases with income for those earning over $120 000 per annum.[8]
BUPA Australia expressed concern that with more expensive policies, the rise in
premium costs from the reduced rebate would only be outweighed by the higher
MLS impost at high income levels. It used Australian Health Insurance
Association (AHIA) data to illustrate the point (see Appendix 4). Assuming an
average single rebate of $1813 per annum (and an average family premium of
$3626 per annum), higher premiums would only exceed the higher MLS impost at
incomes over $120 000 per annum (over $240 000 per annum in the case
of the family).[9]
3.11
The committee recognises that for those in Tiers 1 and 2
($75 001–$120 000), the more expensive the PHI policy, the more that
premium increases—from the lower rebate—will exceed the increase in the MLS if
they were to drop private cover. The AHIA data in Appendix 4 does seem to be
based on fairly expensive policies, however. Even so, it is well to apply
Dr Deeble's observation: a $181 increase in premiums annually (for singles
in Tier 1) is only an extra $3.50 a week for an individual earning well above the
average annual income.[10]
The bills' impact on private health fund membership and the level of cover
3.12
Having considered the effect of the bills' measures on individuals and
families in different income groups, the issue then becomes the extent to which
overall PHI membership will be affected.
3.13
Economists measure the likely effect on consumer demand from a change in
the price a good or service through the concept of 'price elasticity'. Price
elasticities will differ depending on the nature of the good or service in
question. The consultancy, Access Economics, has recently estimated that the
price elasticity of the demand for private health insurance is –0.335.[11]
In other words, a 10 per cent increase in the price of private health
insurance will result in a 3.35 per cent drop in PHI membership.
Treasury's
modelling
3.14
Treasury has
modelled the number of people who are likely to drop their private health
insurance in response to the reduced private health insurance rebate. It estimates
that for Tier 2 ($90 001–$120 000) and Tier 3 ($120 001+), there
will be no net change in PHI coverage.
3.15
Treasury
calculates that for a person aged under 65 in Tiers 2 and 3, the percentage
increase in out-of-pocket PHI costs from the reduced rebate is similar to the
percentage increase in out-of-pocket costs from the increase in the MLS. Table
3.1 shows that for those in Tier 2 ($90 001–$120 000), a 20 per cent
reduction in the PHI rebate represents a 28.6 per cent increase in their PHI
outlay, which is roughly equivalent to the higher MLS (1.25 per cent) if they
drop their policy. Similarly for those earning more than $120 000 (and
under 65 years of age), the increase in out-of-pocket PHI costs (42.9 per cent)
is similar to the increase in out-of-pocket costs from the increase in the MLS
(50 per cent).
Table 3.1: Effect of
higher MLS and lower PHI rebate on Tiers 2 and 3
|
MLS
income range
|
%
increase in out-of-pocket
PHI cost*
|
%
increase in out-of-pocket
MLS cost
|
|
$75,001
- $90,000
$150,001 - $180,000
|
14.3%
|
0%
|
|
$90,001
- $120,000
$180,001 - $240,000
|
28.6%
|
25%
|
|
$120,001+
$240,000+
|
42.9%
|
50%
|
Source:
Treasury, Tabled document, Senate Estimates, 3 June 2009. * This is based on those
currently receiving a 30 per cent PHI rebate (ie: those under 65 years of age)
3.16
Treasury
thereby focused its estimate of those likely to drop PHI in Tier 1 ($75 000
to $90 000). It noted in its submission that it used in its calculations a
price elasticity for private health insurance of –0.2 for those in Tier 1:
for insurees earning between $75 000 to 90 000 per annum, a
1 per cent increase in PHI premiums will result in a 0.2 per cent drop in
PHI membership.[12]
Mr Marty Robinson, Manager of Treasury's Household Modelling and Analysis Unit,
explained how Treasury arrived at the figure of –0.2:
We consulted some of the academic literature about price
elasticities on the basis of observed historical behaviour—of which there is
not much evidence in the public arena. The evidence that we found indicated
some estimates in the vicinity of about minus 0.3 as a price elasticity for
private health insurance...When we undertook our modelling, we felt, however...—that
higher income households are less price sensitive to health insurance and that
in fact incomes are the main driver of people’s decision to purchase private
health insurance. On that basis, we made the decision to discount the assumed
price elasticity for our modelling and assumed a price elasticity of minus 0.2.
So, for example, for every 10 per cent increase in the price of health
insurance for a consumer, we would assume about a two per cent drop in cover in
the affected ranges.[13]
3.17
Treasury then
multiplied this elasticity by the proportional increase in PHI cost for those
in Tier 1 (14.3 per cent: see Table 3.1) to estimate the drop out rate. This
rate was multiplied by the number of singles and couples within the affected
income range.[14]
3.18
On this
basis, Treasury estimates that around 25 000 adults (6500 singles and 5500
couples and families) with PHI cover and earning between the MLS thresholds and
$90 000 (singles) and $180 000 (couples) will opt out of PHI. This
represents a percentage decrease in the number of people with PHI of around
0.26 per cent.[15]
Support for Treasury's views
3.19
Treasury's
estimates have received support from significant quarters. For example, Dr Deeble
has concluded:
...on the
basis of all the Australian and international evidence, that it [the proposed
legislation] will have almost no effect on the underlying structure of the
health care industry. In that respect, I agree entirely with the Treasury's
calculations. People concerned about maintaining the status quo can rest easy.[16]
3.20
Mr Rob Wells,
Director of the College of Medicine, Biology and Environment at the Australian
National University, told the Senate Economics Legislation Committee that in
terms of the bills' effect on drop out from private health insurance:
...all the evidence suggests the impact will be at the low end
of the scale—that is, closer to what the Treasury estimates are, and therefore,
effectively, have a negligible impact I would say on public hospitals and on
premiums. I base my assessment of the situation on a number of factors. First
of all, the reduction in the rebate for high-income earners does not cut out
until singles earn $120,000-plus per annum and families earn $240,000-plus per
annum. That is where you would expect most of the impact to occur because for
incomes below that it is tapered. For those groups, the Medicare levy surcharge
increases quite significantly.
I think the Treasury’s estimate is that the Medicare levy
surcharge and the extra payment because of the reduction in the rebate would
more or less cancel each other out. Therefore, it is only very high-income
earners who would bear the full effect of the measure. We have seen in a
previous budget, the 2007 budget, where the Medicare levy surcharge thresholds
were increased, that people at lower incomes than we are talking about, who
could well have dropped their insurance, did not. In effect, there has been no
reduction in private health insurance since the 2007 budget measure. In fact,
there has been a slight increase.[17]
The Access Economics report
3.21
Catholic
Health Australia commissioned Access Economics to discuss the impact of means
testing the rebate and the related changes to the MLS. A copy of this report
was provided to the Economics Legislation Committee on 11 June 2009.[18]
Its findings were discussed by various witnesses in evidence to the Community
Affairs Legislation Committee.
3.22
Access
Economics was in broad agreement with Treasury's analysis on several key
issues. The report:
-
supported the use of Treasury's personal income tax
micro-simulation model describing it as 'an appropriate tool' for forecasting
the impact of the bills' measures;[19]
-
accepted that 'it is intuitively correct' that higher income
earners will have a lower price elasticity of demand for PHI than the
population generally. On this basis, 'Treasury's assumption does not appear unreasonable';[20]
-
found that 'surcharge avoiders will, for the most part, find it
worthwhile continuing to hold a low cost policy'. This aligns with Treasury's
analysis (Table 3.1) and that of Mr McAuley (Appendix 3); and
-
reached
'broadly the same conclusions' as Treasury regarding the likely fall out from
private health insurance.[21]
3.23
On other
matters, however, Access Economics reserved some caution and doubt for
Treasury's analysis. Most notably, it suspected that Treasury's estimate of PHI
fallout 'may be at the lower end of the range of possibilities' and it 'would
not rule out' a fall in coverage of 100 000 people (from where PHI
membership levels would otherwise have been).[22]
This is because, unlike Treasury, Access Economics factored in a higher price
elasticity for people in Tier 1 than those in the higher-earning Tiers 2 and 3.[23]
3.24
Access
Economics also argued that people in Tier 1 would be most affected by the
bills' measures and would face a net cost of between 25 and 40 per cent.
Although people in Tier 2 could face even larger percentage changes in the net
cost, they are less likely to drop their PHI because their premiums represent a
smaller proportion of their income.
3.25
The Access
Economics report also queried Treasury's not modelling that some PHI fund members
would switch their cover to a lower priced policy. It noted that should this
downgrading occur, there could be greater increases in premiums and 'further
negative impact' on membership levels.[24]
These concerns have been put more forcefully by other organisations (see
below).
Criticism (and counter criticism) of
Treasury's modelling
3.26
The committee
received submissions and took verbal evidence from a few organisations which expressed
concern with various aspects of Treasury's modelling.[25]
Two criticisms deserve particular mention: Treasury's failure to measure the
income elasticity of PHI demand and its failure to model the 'downgrading' of PHI
cover. In both cases, the committee is satisfied with Treasury's approach given
the absence of reliable data and uncertainty as to how people may respond to
the bills' measures.
Income insensitive price elasticity
3.27
In his evidence to the committee, the Chief Executive Officer of
Catholic Health Australia, Mr Martin Laverty, asked rhetorically why Treasury's
estimate of PHI fallout was 75 000 fewer people fewer than the AHIA's
estimate of 100 000. He answered:
It is a very simple explanation. Treasury is assuming that an
income earner on $75,000 a year has the same spending power as an income earner
on some $250,000 a year. Treasury has applied a price elasticity formula to
someone on $75,000 as it has to someone on $250,000. If you think about that
for a moment, it is assuming that, if there is a 10 per cent increase in the
cost of private health insurance for someone on $75,000, that would mean an
average policy is going to be about $2,000. That would represent 3.4 per cent
of the take-home income of someone on $75,000 as opposed to 1.2 per cent of the
take-home income of someone on $250,000.[26]
3.28
Treasury has defended its discounted price elasticity of –0.2.
Mr Robinson told the committee:
The literature upon which we base our price sensitivity is
not available by income level. As I mentioned earlier, the price elasticity of
minus 0.3, which we subsequently discounted to minus 0.2, is basically a broad
estimate of aggregate price sensitivity in the market. Where we do have the
detail within our microsimulation model is in knowing how many taxpayers fall
into each of the income gap categories, broken down by age group as well so
that we can model the impact of the rebate for individual taxpayers on an
aggregate average premium assumption. [27]
3.29
The committee accepts Treasury's position. It highlights Access
Economics' observation in its report for Catholic Health Australia that 'we are
not aware of any specific studies of higher income earners' price elasticity of
demand for PHI'.[28]
Failure to consider 'downgrading'
3.30
APHA, AHIA and
the Western Australian health fund HBF have all argued that Treasury should
have factored into their model the impact of people downgrading their cover and
opting for cheaper policies. HBF's Managing Director, Mr Rob Bransby,
offered anecdotal evidence that in response to the bills:
...people will be looking at the whole proposition and will be
looking at every opportunity to downgrade. If you do not see value in
ancillary, for example, and you are in that middle-income bracket, you would
probably struggle to find value and maybe you would self-insure. I would also
suggest that if you did get a substantive increase on an already relatively
expensive product you would look at the proposition again to see whether you
could take some cost out of it.[29]
3.31
APHA's Chief
Executive, Mr Roff, also indicated that in contrast to the Treasury's
assumptions, the 'rational' response to higher premiums will be for people to
adjust their PHI cover:
They [Treasury] have assumed that people will either keep
their insurance or drop their insurance and there will be no other decisions
made, where obviously a rational decision would be to try and lower the
premium. There are two key ways that that can happen: either by taking out a
front-end deductible or an excess, or by taking a policy with exclusions that
does not provide benefits for treatment of particular services. Both of those
cause problems for my members.[30]
3.32
AHIA's Chief
Executive Officer, Dr Michael Armitage, told the committee:
...we are very fearful that...the biggest effect of this
legislation...will actually be people downgrading their cover, because again
people can downgrade with no Medicare levy surcharge penalty. If the argument
is, ‘This will happen because we have increased the stick,’ if people can take
what is a legitimate financial decision in difficult financial times without
the stick being there, we think logically the government must acknowledge that
there will be a lot of people who will downgrade.
...
We think that the downgrading is a major effect. For Treasury
not to model it is disingenuous because it just does not reflect the reality of
what is going to happen.[31]
3.33
AHIA supported the survey-based opinion polling process arguing that
this is a superior tool to the Treasury modelling. AHIA has estimated the
number of people likely to downgrade their cover based on IPSOS and Roy Morgan
surveys. Dr Armitage explained that the surveys give an income spread for
those with private health insurance and indicate the intent to leave and
downgrade PHI.[32]
AHIA's submission noted that 730 000 people with private hospital cover
are likely to downgrade their cover and 775 000 people with private health
cover are very likely to exit their ancillary cover.[33]
3.34
In evidence to the committee, Dr Armitage defended the
integrity of these surveys. He
contrasted this approach with Treasury's methodology:
...Treasury has modelled with a computer chip what it thinks
might happen. We have actually gone out and asked people, through the Ipsos
survey and through Roy Morgan et cetera: what will you do if your private
health insurance cover increases by X per cent? We know what people will do
because of that.[34]
3.35
This confidence was not shared by Catholic Health Australia. In his
evidence to the committee, Mr Laverty emphasised that it is uncertain the
extent to which those with PHI might downgrade:
...the only opportunity we have had to scrutinise their [Treasury's]
numbers is around the level of price elasticity that Treasury has applied, and
that does not give consideration to this much larger prospect of downgrading
and what it means for out-of-pocket costs. I think it is quite important to consider
that we are likely to see more consumers complaining about the out-of-pocket
costs or the gaps that they are likely to pay. We have not been able to assess
what that impact will be and Treasury has not been able to assess what that
impact will be. It is an uncertainty, and in that context we would ask: if it
is that uncertain, should we support this particular measure?[35]
3.36
Treasury explained at a Senate Estimates hearing in June 2009 that it was
unable to model the effects of the rebate changes on General Treatment cover as
it does not have the income data for those who hold ancillary cover
exclusively.[36]
It noted at that hearing, and again before this committee, the Treasury's view
that the majority of people with ancillary cover would be under the Medicare
levy threshold (currently set at $70 000).[37]
3.37
Still, Mr Robinson told the committee that in the absence of
reliable data:
...there is a lot of uncertainty. The private health insurers
themselves do not, as you have mentioned, have income information for their
members. There is no empirical evidence based on observed behaviour which
estimates any price elasticity for people downgrading health cover. That is not
to say that it will not happen, but...there are in the order of 20,000 health
insurance products out there and the government’s policy may induce people to
reassess the policy they currently have.[38]
3.38
Dr Deeble also questioned the availability of a reliable data
source to measure downgrading:
...Treasury has not considered downgrades...But I cannot see how anybody
else could assess what the downgrades might be. They have no data on people’s
incomes. They have done some surveys, I am sure, but I am quite certain that
the question was asked in such a way that the person would have thought that
they were going to lose all their rebate and not just a little bit. I think
there is an effect that is not calculated, but I do not know how anybody would
do it and I would not say that that should be a reason for deferring the whole
consideration on the possibility that some people might downgrade their cover.[39]
3.39
Mr McAuley told the committee that under both the existing and the
proposed systems, there is an incentive to downgrade cover (to buy a cheap
policy for less that the MLS). He notes that despite the incentive to downgrade
currently in place, 'people are not doing that'.[40]
3.40
The committee shares doubts as to the accuracy of market research in
gauging the likelihood that people will downgrade their PHI cover. It disputes
the claims that downgrading 'will happen' and that it should therefore have
been modelled.[41]
Behavioural
observations
3.41
The preceding
discussion on the likely impact of the legislation has noted that while the rational
response to higher premiums is to drop or downgrade PHI cover, this will not
necessarily be the case. Indeed, it would be wrong to suggest that those who
hold PHI do so solely based on comparing the cost of premiums with the cost of
incurring the surcharge. Surveys show that people buy private health insurance
for a variety of reasons. The 2007–08 National Health Survey found that
'security, protection and peace of mind' was the most common reason for having
private health insurance (54 per cent of those insured).[42]
Interestingly, the category 'cannot afford it/too expensive' was the most
commonly reported reason for not insuring (58 per cent of those without private
health insurance).[43]
Inertia—overinsurance and the 'endowment
effect'
3.42
Mr McAuley,
while observing the bills' incentives for people to take up and to downgrade
their cover, argued that 'there will be little change in PHI coverage,
and similarly not a great deal of switching to lower price policies'.[44]
He cited several reasons for this 'inertia' including tendencies for people to
'hang on to' what they have (the 'endowment' effect) and for higher income
groups to overinsure:[45]
Even though there is very good behavioural research and even
though theoretically those who have more wealth should need less insurance
because they can cover more of their own risks, the reality is that those with
more wealth take more insurance and tend to cover themselves to the hilt.[46]
3.43
Mr Wells told the Senate
Economics Legislation Committee that DoHA had suggested in recent evidence at a
Senate Estimates hearing that most people who hold private health insurance
now hold it because they want to hold it. He added: 'that makes it even less
likely that people will drop it simply because of some rearrangement of
surcharges and levies'.[47]
3.44
A related aspect of private
health insurance is that it is more sensitive to income than to price. Dr
Deeble wrote in his submission that richer people are more likely to hold private health insurance
than poorer people and changes in income have a significant affect on
membership.[48]
He added:
It is, in fact, almost impossible for people to understand
all of the various products that the health insurers offer and decide whether
they represent value for money. That is not to say that price would never be
important, only that people buy private health insurance for a variety of reasons,
including custom, amenity, perceptions of social position and concerns about
the availability and quality of the public alternative. Both the statistical
evidence and practical experience suggest that cost is rarely the dominant
factor and that, for the highest income groups, even quite large variations are
irrelevant.[49]
3.45
Dr Deeble told the committee that Treasury's estimate of price
elasticity (-0.2) 'may even be a little high'.[50]
He told the committee that based on his experience on the board of Medibank Private:
...we could vary up to 10 to 15 per cent away from our
competitors with no marked effect on our market share; and when we all raised
prices, together or separately, we lost no market share and the total market
share did not vary...I can confirm from personal experience that the effect price
on demand and market share for any individual company or the whole industry is
very, very low indeed—it has very little effect.[51]
Historical
observations
3.46
Two
historical observations add to the argument that the drop out rate from means
testing the PHI rebate will be relatively small. First, that given a third of
the population was privately insured prior to the introduction of the 30 per
cent private health insurance rebate (Chart 3.1), it seems likely that many (if
not most) of those people will retain their cover even if the rebate is
withdrawn completely. Indeed, as Mr McAuley told the committee:
...since 1999 the increases in private health insurance, in
real terms, have wiped out the original 30 per cent rebates, yet there has been
no significant net change. So empirically we find that people do hang on to
insurance in spite of what has been in the order of a 40 per cent rise in real
terms, inflation adjusted.[52]
3.47
The second
historical observation is that fund membership levels did not increase markedly
in response to the 30 per cent rebate in early 1999 (Chart 3.1). Why, then,
would partial withdrawal of the subsidy lead people to drop their cover? The
significant increase in membership between the December 2000 and December 2001
quarters is widely attributed to the 'Run for Cover' campaign in the lead up to
the 1 July 2000 introduction of the Lifetime Health Cover initiative.[53]
Indeed, the Australian Healthcare and Hospitals Association has argued that in
light of this experience, Lifetime Health Cover is the 'main measure that would
have any impact on hospital usage'.[54]
Chart 3.1: Proportion of
population (per cent) with PHI, 1997–2008
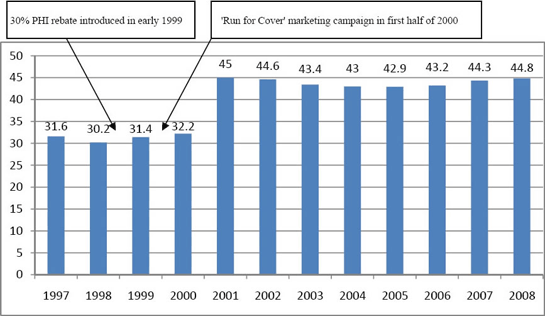
Source: Private Health
Administration Council, Part A Report, March Quarter 2009.
Figures are for December quarters. The data is reproduced from a table
presented in Submission 1 by Dr John Deeble.
3.48
The influence
of the 2000 'Run for Cover' marketing campaign suggests that the impact of this
legislation on insurance levels will largely depend on the information that
people receive. In anticipation of this legislation being passed, some health
funds and health insurance brokers have conducted marketing campaigns
encouraging people to take up private health insurance lest they should have to
pay 'an extra 1% in tax'.[55]
This may persuade some people to take up, or at least remain in, a private
fund.[56]
3.49
However, many
people will be either unaware of the changes or disinterested in them. As Dr
Deeble noted during last year's Senate inquiry into the MLS thresholds, a
combination of 'ignorance, apathy and uncertainty' will potentially limit the
immediate fallout from the funds.[57]
The same could be said of these bills' measures. Insurees would need to know
their taxable income and calculate the likely increase in their premiums from a
lower rebate relative to the increase they would incur in the surcharge if they
dropped their insurance. It seems unlikely that too many accountants will
advise their clients to drop their PHI. Treasury's calculations support this
view (see Table 3.1).
The impact on the
public (and private) hospital system
3.50
The committee
received evidence expressing concern that the fallout from private health
insurance as a response to the lower rebate would place pressure on the public
hospital system. This would be exacerbated as premiums increased in response to
the initial loss of members, causing further loss of members and greater reliance
on public hospitals. This pattern is known as the 'second and third round
effect'.
3.51
Mr Mark
Engel, Director of Marketing at BUPA Australia, explained the likely impact on
the public hospital system of those who leave PHI or downgrade their cover:
The impact of these decisions by customers will be felt in
two ways: firstly, those people who downgrade or drop will increasingly rely on
the already stretched public sector for their health care needs, which are no
longer covered by their health insurance; and, secondly, it has the potential
to price choice in health care beyond the reach of low to middle income
earners. Those Australians who are forced to drop their health cover for
financial reasons will be forced into a public system under greater pressure
with even longer waiting lists.[58]
3.52
AHIA argued
that based on its market research, 'up to 240,000 Australians with private
hospital insurance are likely to exit their cover as a result of this
legislation'.[59]
In terms of the impact of the bills' measures on the public hospital system,
AHIA estimated:
...a loss of almost 75,000 episodes from the private sector,
representing nearly 190,000 bed days a year. The transfer of these procedures
to the public hospital system reflects an additional annual cost burden of $195
million on State and Territory governments, as more Australians exit their
private cover to depend solely on the public system for care.[60]
3.53
Catholic Health Australia told the committee that based on AHIA's survey-based
estimate of 100 000 people exiting PHI, it anticipated 36 000 people
joining public hospital waiting queues. Forecasts aside, Mr Laverty told the
committee that:
...any pressure on public hospital waiting lists is an unwanted
one, and why would we be taking a risk without putting in place a safety net, a
monitoring mechanism or a compensation arrangement to ensure that those public
hospital waiting lists are not increased? That is the principal concern that I
put before this inquiry. Because we have a foot both in private hospitals and
in public hospitals and because the mission imperative of Catholic hospital
services in Australia is ultimately for low-income earners, for those poor and
marginalised, any pressure on public hospital waiting lists is not something
that we would be comfortable with.[61]
3.54
Mr Laverty told the committee that at a minimum, the government should
commit to monitoring the impact of the legislation on public hospitals. And if
necessary, he argued, there should be a 'compensatory measure' through the
health care agreements to the states and territories.[62]
3.55
The committee notes that an ex post facto analysis to isolate the effect
of the legislation on public hospitals would be highly complex. As Ms Penny
Shakespeare, Assistant Secretary of DoHA's Acute Care Division, told the
committee:
It is also very difficult to work out what the impact would
be on public hospitals because everybody who is eligible for Medicare is
entitled to be treated as a public patient in a public hospital whether or not
they have private health insurance and whether or not they have comprehensive
private health insurance. It would be quite difficult for us to tell if
somebody were presenting to a public hospital because this measure had resulted
in them taking out a product with an exclusion or whether they would have
decided to be treated as a public patient anyway.[63]
Treasury and DoHA's view
3.56
In evidence
to the committee, Treasury explained that it was not required under the Charter
of Budget Honesty to model the second and third round effects.[64]
These effects include the impact of the measures on the use of public
hospitals.
3.57
In its submission to
this inquiry, the Department of Health and Ageing (DoHA) noted that the
legislation will lead 40 000 people to drop their private health cover,
resulting in an extra 8000 public hospital visits or 'episodes'. The figure of
40 000 people comes from 25 000 who are expected to drop their
hospital and/or general treatment cover, 10 000 who will keep their
hospital cover but drop their general treatment cover and 5000 who have a
general treatment policy only and drop that cover.[65]
3.58
This rate of
PHI cover to public hospital 'episodes'—roughly 3 to 1—is corroborated by
Catholic Health Australia's estimates.[66] Access Economics also accepts
Treasury's analysis that if the drop out figure is 25 000 adults, then the
impact on public hospitals will be roughly 8000 'episodes'. It also recognised
that some privately insured patients now use the public system (as private
patients). If they drop their cover, the effect on public hospitals is a loss
of revenue rather than extra cost associated with extra volume.[67]
Other
views on the impact of the bills on public hospitals
3.59
Several submitters
to this inquiry downplayed the effect that the government's measures may have
on the public hospital system from a fall in PHI membership. Mr Wells told
the Senate Economics Legislation Committee that if people keep their cover and
drop their hospital cover there would be no impact on the public hospital
system because 'ancillary cover does not cover the sorts of things you
get in a public hospital'.[68]
3.60
Mr McAuley
has argued that the support given to private health insurance over the past
decade has had the effect of shifting resources—surgeons, nurses, etc.— to the
private sector. It has not taken pressure off the public system because it has
taken these scarce resources away from public hospitals and to the private
sector.[69]
Private hospitals, financed heavily by the private insurance funds, tend to
offer a limited range of elective surgeries and tend to over treat patients.[70]
Mr McAuley noted that the private funds cannot achieve effective cost
control because the service providers will seek out those insurers willing to
cover the higher cost. The same problem has been observed internationally.[71]
3.61
Access
Economics has noted that the impact of the measures on the public hospital
system will depend on an assessment of those most likely to drop their cover.
Intuitively, this group will be a combination of those least likely to need it
and those least able to afford it. The impact will be minimal if the drop outs
are concentrated among 'surcharge avoiders' who are in PHI for monetary reasons
and attach little or no value to any potential fund benefits. On the other
hand, the impact on public hospitals may be substantial if those who leave the
funds are among the older, high service using cohort.
Committee view
3.62
The committee
agrees with Treasury that the impact of the bills' measures on private health
fund membership, and any subsequent impact on public hospitals, will be
relatively minor. It emphasises that the bills will only impact directly on the
wealthiest quartile of those with private health insurance. This reflects the
rationale for the legislation: that those who have the capacity to pay for their
PHI should properly do so from their own pocket. In terms of whether this
cohort will drop or downgrade their cover, the behavioural evidence indicates
that not only do the wealthy overinsure, they place high value on retaining
this cover. Private health insurance is more responsive to income than to
price. For these reasons, the committee believes that the legislation is fair
and largely undisruptive.
3.63
To the extent
that those on higher incomes do downgrade their policies, the committee
believes the legislation will promote an equitable adjustment. Those with PHI
(often on higher incomes) are currently subsidised through the 30 per cent
rebate for their ancillary treatment, while those without PHI (often on lower
incomes) pay for this treatment without any taxpayer assistance. However, the
committee thinks that in the absence of a significant marketing campaign, it is
unlikely that many people will drop their ancillary cover.[72]
3.64
The committee
has not had the benefit of assessing the methodology of the AHIA-commissioned market
research. It does emphasise, however, the well-known limitations of this type
of approach which is heavily dependent on question format.[73]
How people respond to the prospect of higher premiums in a survey will often
differ to how they respond in practice.
3.65
More
particularly, the committee queries AHIA's assumption that there will be a
direct and absolute transfer of private hospital 'episodes' to the public
system. It highlights research indicating the over treatment of patients in
private hospitals and the fact that private hospitals offer many treatments
which are non-essential and may be forgone. Many people with private insurance
are already treated in public hospitals and some of those who drop their
ancillary cover will self insure in a private hospital.
The process of
implementing the means tested rebate
3.66
In its tabled
opening statement to the committee, DoHA gave several examples as to how a
person might claim the rebate under the proposed means testing arrangements.
3.67
A person (or family)
with PHI in the affected income range (>$75 000) can advise their
insurer to deduct a lower rebate level from their premium. The person would
nominate his/her new rebate level according to their income and age (although
they need not provide these precise details to their insurer). The insurer
would reduce the premium charged by the lesser rate (either 10, 20 or 30 per
cent). The share met by the Government—through rebate payments provided by
Medicare Australia directly to the insurer—would be reduced accordingly, and
the insuree would pay a higher a premium to cover the lower rebate.[74]
3.68
Alternatively,
a person could decide not to inform the insurer of their details. In this case,
s/he will continue to receive the 30 per cent rebate (or higher if they are over
65 years). Having been overpaid for the rebate, the person will incur a tax
debt of the amount for which they were overcompensated.[75]
3.69
A third
option is to change the way the rebate is claimed. If a person is unsure of the
income they might earn in a given financial year and did not want to incur a
tax liability, they could advise their insurer not to deduct any rebate from
their premium payments. The appropriate rebate could then be claimed through a
tax return. This option of claiming the rebate as a tax deduction already
exists.[76]
3.70
A fourth
possibility is to claim the rebate as a refund at a Medicare office. In this
case, a person pays their PHI premium on a quarterly basis and claims the full (non-means
tested) rebate at the Medicare office. If his/her income for that year exceeds
the amount eligible for the full rebate, the difference between the rebate
claimed and the rebate to which they are entitled would be repaid as a tax
debt.[77]
Concerns with the proposed process
for means-testing the rebate
3.71
The committee
has received comment that means testing the private health insurance rebate may
create uncertainty for consumers and complexity for administrators. Dr Deeble,
for example, qualified his support for the bill by commenting: 'like all means-tested
arrangements, the system will be more complex to administer than at present'.[78]
Various organisations have voiced their own concerns.
3.72
The AHIA has
expressed its fear that:
...additional burdens will be placed on our Fund Members as
part of the implementation and administration of this legislation. A briefing
to Industry from the Department of Health and Ageing following the Budget
announcement suggests that Private Health Funds will be required to request
that fund members self‐identify
which rebate level they are entitled to, before their eligibility is then
reconciled by the Australian Taxation Office as part of the individual’s annual
tax assessment. This process is likely to lead to confusion amongst policy
holders as to their entitlement if their income level varies from year‐to‐year and will also add
cost imposts on Private Health Funds as they implement new systems to
accommodate the policy change.[79]
3.73
In its submission to this inquiry, BUPA Australia commented:
For the industry, the lack of clarity around administration
of the scheme means the costs of start-up, systems, communication and ongoing
administration of this far more complex proposed rebate scheme cannot be
estimated. This is of considerable concern, as we are still unclear on the degree
to which these costs could ultimately impact on our customers through their
premiums. The proposed changes will...serve to increase complexity for a very
large number of PHI customers. To ensure this is managed as smoothly and
effectively as possible, the Federal Government should commit to a significant
annual consumer communications campaign, incorporating mailings and production
of printed material and forms.[80]
3.74
The Health Insurance
Restricted Membership Association of Australia (HIRMAA) has also expressed
concerns with the administration of the means tested rebate. In particular, it
stressed that no health insurers are expected or obliged to act as agents of
the Australian Taxation Office (ATO) and consumers must be able to access their
rebate through an upfront deduction by the insurer, through a Medicare office
or through their tax return.[81]
3.75
DoHA assured the committee that the administrative cost to insurers from
implementing the incentive tiers would be minimal. Ms Shakespeare told the
committee that the major cost to the funds would be to change their systems to
recognise the additional rebate tiers. She noted that the funds have had
experience in this process when the previous government a higher rebate for
higher age groups.
We have actually had a look back to see what happened last
time we introduced additional rebate tiers that their systems needed to
recognise...in 2005. For premium submissions made in that year no insurer
mentioned additional administrative costs associated with the introduction of
the additional rebate as a reason for additional premium increases. In fact,
management expense ratios decreased.[82]
3.76
The Government
has in place plans to deal with all these issues. When claiming the rebate as a
premium deduction or through a refund at Medicare, a person will need to
nominate a premium rebate level that they are entitled to based on their
'adjusted taxable income'. If they over-estimate their income, they will
receive a rebate refund through their tax return for that year; if they under-estimate
their income, they will incur a rebate debt through their tax return which will
be recoverable as a normal tax debt.[83]
3.77
DoHA's
submission also noted that funding for a communications campaign about the
changes has been provided to the ATO through the 2009–10 budget. It will be
coordinated by the ATO with support from DoHA. DoHA will concentrate its
efforts on assisting industry to implement the changes through the development
of 'information and guidance material'.[84]
Committee view
3.78
The committee is satisfied that the Government has set aside adequate
funding and resources to inform and instruct the industry and the public as to
how the means tested private health insurance rebate will operate.
Recommendation
3.79 The committee recommends that the bills be passed.
Senator Claire
Moore
Chair
August 2009
Navigation: Previous Page | Contents | Next Page